- What are kidney stones (urinary calculi)?
- Symptoms of Kidney Stones
- Diagnosis
- Laboratory Evaluation
- Radiologic Evaluation
- Treatment of Kidney Stones
Miami urologists David Robbins, MD and Amery Wirtshafter, MD specialize in the minimally invasive treatment of kidney stones. Using the state of the art technology, our board-certified urologists have the specialized training and skills necessary to assist patients even with complex stones to become stone-free with minimal impact on their daily lives. When choosing a urologist to treat kidney stones, it is highly recommended to seek urologists such as Dr. Robbins and Dr. Wirtshafter who specialize in kidney stone diagnosis and treatment to maximize your probability of a successful outcome and avoid complications of kidney stone treatment. When it comes to improved outcomes following surgery for kidney stones, experience does matter. Please call our Miami office today to schedule an appointment with one of our kidney stone treatment specialists.
What are kidney stones (urinary calculi)?
Kidney stones (urinary calculi) are stones formed from concentrated levels of minerals typically found in the urine such as calcium and uric acid. If these minerals concentrate to high enough levels they will crystallize and accumulate into larger stone-like structures known as urinary calculi. They can form anywhere in the urinary tract from the kidneys down to the ureters and bladder. The most common type of stone is made up of calcium oxalate followed in order of decreasing frequency by uric acid, infectious stones known as "struvite" stones, and cystine stones. Urinary calculi can range in size from just a few millimeters to several centimeters occupying the entire collecting system of the kidney. Kidney stones are responsible for a tremendous burden to society equaling billions of dollars a year in health care costs and missed workdays.
Symptoms of Kidney Stones
When a kidney stone drops down from the kidney to the bladder it may get caught in the ureter producing a sudden and severe pain in the side radiating toward the groin known as "renal colic". The pain that a patient experiences from kidney stones are caused by the obstruction of urine trying to pass down the ureter from the kidney to the bladder. As the urine builds up behind the level of the obstructed stone, it puts pressure on the kidney resulting in severe and incapacitating pain often associated with nausea and vomiting. Patients passing kidney stones may present with other symptoms including blood in the urine known as hematuria which may be visible with the naked eye or only seen under the microscope. If the urine behind the stone becomes infected it may manifest as fever and can lead to sepsis and even death if the obstruction is not relieved by a stent or a percutaneous nephrostomy tube.
Diagnosis
The diagnosis of kidney stones is often made by history and physical exam alone given the classic presentation of many patients including sudden onset severe flank pain radiating to the groin, nausea vomiting, and tenderness to palpation on the flank. Patients with a past medical history including prior urinary calculi, gout, hyperparathyroidism, diabetes, obesity, inflammatory bowel disease, renal tubular acidosis, and gastric bypass surgery have an elevated risk for stone disease. A patient passing a stone typically appears restless and is unable to find a comfortable position resulting in relief of their pain.
Laboratory Evaluation
Typical laboratory evaluation for a kidney stone includes a complete blood count, basic metabolic panel, urinalysis, and urine culture. An elevated white blood count may indicate that an infection is brewing. The patient's creatinine provides an estimate of his or her overall kidney function which may be impaired from obstruction of the kidney caused by the passing stone or dehydration caused by an inability to tolerate oral fluids and/or vomiting. A urinalysis may show red microscopic or grossly apparent red blood cells that are released as the stone causes abrasion of the wall of the kidney or ureter as it passes down into the bladder. A urine culture is important in the event of an infection to be able to later tailor antibiotic therapy to a specific bacteria subtype in the event of an infection.
Patients with recurrent stone disease or first-time stone formers in whom passing another stone can be very dangerous such as airplane pilots require further evaluation to determine the metabolic abnormality that may be causing them to form stones. A typical metabolic evaluation includes sending any passed or treated stone for evaluation to determine its chemical composition, a 24-hour urine evaluation including calcium, uric acid, oxalate, magnesium, phosphorus and citrate, and blood tests including calcium, uric acid, potassium, and sometimes parathyroid hormone. This important workup can guide the physician to prescribe medications that can decrease the risk of stone formation in the future. Regardless of the etiology for stone formation, all stone formers are encouraged to increase their fluid intake until they are expelling 2-3 liters of urine daily and to decrease their intake of salt and meat of any kind.
Radiologic Evaluation
CT scan (Computed Tomography Scan)
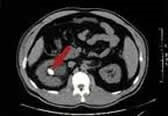
The most valuable tool in making a definitive diagnosis for a passing stone is imaging. A non-contrast CT scan has become the gold standard test for evaluating stone disease. A CT scan is used to obtain cross-sectional images of the patient's abdomen and pelvis. A stone typically shows up bright white in the urinary tract allowing the physician to understand exactly where the stone is located from the kidney down the ureter to the bladder as well as the size and shape of the stone. Based on a radiological measurement known as Houndsfield units, the physician can estimate the density of the stone and even potentially determine the stone's composition. For example, a uric acid stone which is typically less dense often has a Houndsfield value below 400 HU. This information is important because uric acid stones are one of the only stones that can be treated with medical therapy to dissolve them.
KUB (Kidney-Ureter-Bladder X-Ray)
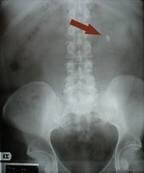
A KUB (Kidney-Ureter-Bladder abdominal x-ray) is another radiographical tool used by physicians to evaluate for stones. Although a KUB does not provide the detailed anatomic information available in a CT scan, it is certainly an important tool in that it exposes the patient to less radiation than a CT scan and can be used to see if a stone is passing further down the ureter allowing the patient and physician to feel more comfortable continuing with conservative management of a stone that is passing rather than proceeding with operative intervention. Uric acid stones are not seen on a KUB and this information is important because a stone that cannot be seen with an X-ray can typically not be treated with ESWL (Extracorporeal Shock Wave Lithotripsy).
Ultrasound
Renal ultrasound is a useful test because it allows the physician to view stones in the kidney and determine if their size and position without exposing the patient to radiation or intravenous contrast dye. Additionally, a dilated collecting system or renal pelvis is seen on a renal ultrasound is a secondary indicator of a passing stone. Unfortunately, ultrasound is not very sensitive for visualizing stones in the ureter or to confirm that a stone has passed.
Treatment of Kidney Stones (Kidney Stone Removal)
Patients with kidney stones in the prior generation commonly underwent large open surgeries for the treatment of even small passing stones. They required days to weeks of recovery time in the hospital and were often left with large unsightly scars and chronic incisional pain. Nowadays the need for open surgery for kidney stones is extraordinarily rare. Modern technology such as high-resolution CT scan, holmium laser lithotripsy fibers less than a millimeter in thickness, high definition endoscopic cameras, and extracorporeal shock wave lithotriptors allow urologists to treat even large complex stones with a high probability of complete stone clearance without the need for open surgery.
Conservative Management of Kidney stones
Kidney stones can oftentimes pass spontaneously without the need for surgical instrumentation of any kind. On average, stones 3-5 millimeters in size have between a 50-80% chance of passage down the entire length of the ureter without the need for intervention. When a stone reaches 8mm, however, the chance of spontaneous passage begins to drop dramatically. To assist patients to pass a stone, urologists will often recommend increasing oral hydration and will recommend pain control with NSAIDs such as Ibuprofen or narcotic pain medication. Sometimes patients will be admitted to the hospital for hydration with IV fluid and strong pain medication to assist with the stone passage. Recently the use of alpha-blockers such as tamsulosin (Flomax) is prescribed to patients passing stones. This medication significantly increases the rate of spontaneous stone passage likely to be a way of relaxing the smooth muscle in the wall of the ureter. If a patient passing a stone develops a fever, conservative management must be aborted and a patient will need an emergent stent placement or nephrostomy tube to relieve the obstruction and prevent sepsis. Other more relative indications to abort conservative management include intractable pain or inability to keep down food and water due to persistent nausea and vomiting.
Surgical Interventions for Kidney Stones
When conservative measures fail or if a stone is too large to reasonably pass, surgical intervention may be recommended. There are numerous minimally invasive methods used to treat stones which are outlined below.
Ureteroscopy and Holmium Laser Lithotripsy
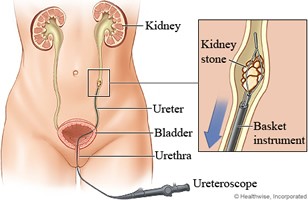
Ureteroscopy and holmium laser lithotripsy is typically indicated for the treatment of obstructing ureteral stones greater than 5mm in size or for stones in the kidney less than 2cm in size. Stones located in the lower pole of the kidney are more difficult to treat and so stones greater than 1cm in size in this location can be moved with a basket to a more favorable location or treated with an alternative method whether it be PCNL (Percutaneous Nephrostolithotomy) or ESWL (Extracorporeal Shock Wave Lithotripsy). Ureteroscopy to remove kidney stones is typically performed under general anesthesia as an outpatient procedure. A ureteroscope which is a long narrow camera or telescope is introduced into the urethra and up the ureter. When the stone is visualized, it is fragmented into tiny easily passable pieces using a narrow holmium laser fiber. A flexible plastic tube is then left in the ureter for a week or two to allow for passive dilation of the ureter to assist in the passage of the tiny stone fragments. In skilled hands, this procedure can be used to treat obstructing ureteral stones with a high degree of success with operative times under an hour.
Extracorporeal Shock Wave Lithotripsy (ESWL)
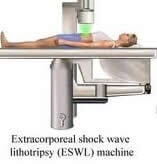
ESWL is a minimally invasive technique that employs an energy source known as a lithotriptor that uses shock waves generated outside of the body to fragment kidney stones. These stones then must pass spontaneously down the ureter. Occasionally a urologist may place a stent at the time of ESWL to assist in the stone passage. Real-time X-ray known as fluoroscopy is used to locate the stone and focus the shock wave. Stones that are less dense and not seen on X-ray such as uric acid stones are not able to be treated with ESWL.
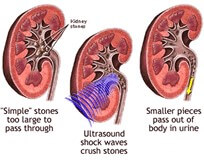
ESWL is typically used to treat non-obstructing kidney stones less than 1-2 cm in size. ESWL is less successful for more dense stones such as those composed of calcium oxalate monohydrate or cystine. ESWL is directly contraindicated for patients with an obstructing stone and fever or infection. ESWL is performed as an outpatient procedure with operative times around 30 minutes.
Percutaneous Nephrolithotomy (PCNL)
Percutaneous Nephrolithotomy (PCNL) is an excellent modality of therapy for the treatment of kidney stones greater than 2cm in size, staghorn calculi, large lower pole stones, or patients with anatomic abnormalities of the kidneys precluding treatment with ureteroscopy.
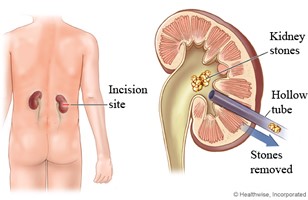
PCNL is a more invasive method of treatment and removal of kidney stones involving creating an access point into the kidney via the skin through a patients' flank. A larger access sheath is placed into the kidney allowing the passage of a larger camera (nephroscope) and stone fragmenting devices. Using PCNL, the goal is to completely fragment large stones and pull all of the pieces out of the access sheath so that they do not have to pass down the ureter. A nephrostomy tube is commonly left at the end of the procedure to allow maximum drainage of the kidney. General anesthesia is used and a patient may have to spend 1-3 days in the hospital to recover.
Request Your Consultation Today!
To request your consultation, please call (305) 575-2771 or contact us online today!
Our Locations
12411 Biscayne Boulevard
North Miami, FL 33181
Phone: (305) 575-2771
Get Directions






